 8686 139 139
8686 139 139
 8686 139 139
8686 139 139
Caring for individuals with mental health concerns can be challenging, mainly because these conditions are often less understood compared to physical ailments. Unlike physical diseases that are typically easier to diagnose and treat, mental health conditions can be more complex and are sometimes harder to define. Their symptoms can vary widely and may not be visible to others, making it difficult for people to empathise and offer appropriate support. This gap in understanding can lead to misunderstandings and a lack of compassion.
We encourage you to educate yourself about the specific mental health disorder your care-recipient is experiencing. Understanding the condition, its symptoms, treatment options, and prognosis can significantly improve your ability to respond effectively. This knowledge will also enable you to identify concerning changes in their behaviour or mental state, prompting you to seek professional help when necessary.
Below are some mental health concerns and corresponding caregiving support strategies:
To help a caregiver recognise patterns in mood fluctuations, common triggers, and the progress made by their care-recipient, we recommend using a daily mood tracker. This tool can help prioritise activities that positively influence the care-recipient's well-being and prepare the caregiver for times when they need to seek assistance. Additionally, a mood tracker can serve as a reference when discussing concerns and challenges with a professional.
For a care-recipient who may struggle to express their emotions, a mood tracker is valuable for documenting their feelings. This tool enhances a caregiver's ability to respond to emotional needs, thereby providing more compassionate and effective care.
Below is a table that can be used to note the care-recipient's emotions, activities, and triggers.
| Mood rating for the day (using the scale): | Morning | Noon | Evening |
|---|---|---|---|
| Activities and associated emotions | |||
| Triggers |
Mood rating: Mark the care-recipient's mood on the scale given below, where 10 represents being extremely joyful/energetic, and 1 indicates being extremely depressed/hopeless. Whenever possible ask the care-recipient about their mood and let them decide what they are feeling. Try not to make assumptions.
| Rating | Description |
|---|---|
| 1 | Extremely depressed, feeling hopeless. |
| 2 | Very low mood, overwhelmed and drained. |
| 3 | Sad and struggling, little motivation. |
| 4 | Low mood, anxious, feeling disconnected. |
| 5 | Neutral, neither happy nor sad. |
| 6 | Mildly low, restless or slightly anxious. |
| 7 | Stable mood, generally calm and content. |
| 8 | Good mood, feeling positive and energised. |
| 9 | Very happy, optimistic, and full of energy. |
| 10 | Extremely joyful, feeling on top of the world. |
Activities and associated emotions: Keep a daily log of significant activities that occur throughout the day, along with the emotions experienced by the care-recipient during those activities. For example, you may note, “taking a walk (felt happy),” “meeting up with a friend (felt excited and playful),” or “attending doctor’s visit (felt scared).” You can refer to the emotional wheel to identify the emotion that resonates the most when doing that activity.
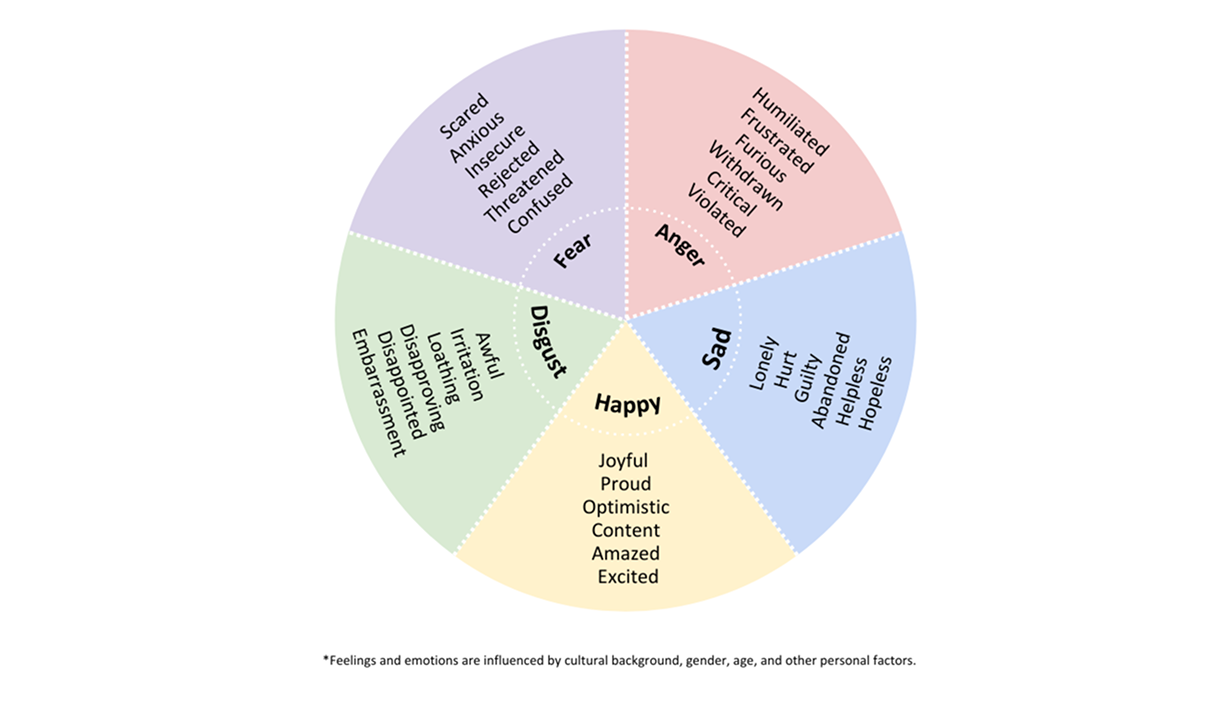
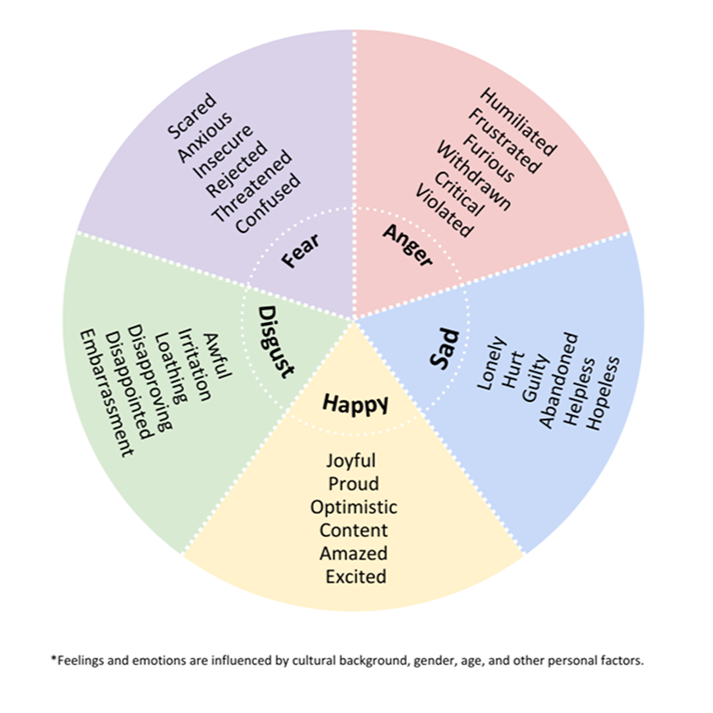
Triggers: Note down if there are any stressors that disrupt your care-recipient’s mood or evoke a powerful response. For example, it can be something as simple as getting annoyed when the food doesn't arrive on time.
Professional guidance can provide more comprehensive support. Feel free to share the contact information for our Free Counselling Helpline service with your care-recipient. Our helpline number is 8686139139, and operates every day of the week from 9am to 8pm. Additionally, to receive 1-to-1 appointment based online therapy, they can book the session by clicking on link.
Bipolar disorders are characterised by fluctuations in the mood ranging from high and elevated (mania) to low and depressed (depression).

Early detection: Tracking your loved one's mood regularly can help predict when a manic or depressive episode may occur. Regularly tracking these mood changes can help you plan interventions and support them.

Consistency is key: Bipolar disorder is most effectively managed when medication is taken consistently. However, a care-recipient may forget or skip doses during a manic episode, as they may want to continue experiencing high energy. Conversely, during a depressive episode, they may feel too exhausted to prioritise their medication.

Use energy positively: Instead of trying to calm your loved one during a manic episode, channel their energy into fun and productive activities, such as starting a painting project or writing.

Limit risky behaviour: Set clear boundaries around impulsive decisions, like overspending or overcommitting to events. For example, create a budget, or limit the number of activities or keep the credit card or phone away (if discussed previously). This can help prevent the excitement from turning into risky behaviour, keeping the situation enjoyable and safe.

Helpful statements for manic episodes: “You seem full of energy! Let’s start a painting project together; it could be fun!”
“I see you are excited about planning events. How about we choose just one event to attend this weekend? We can make it special!”
“It sounds like you want to buy some new things. Let’s set a small budget for shopping to keep it fun and safe.”

Offer emotional support: During depressive episodes, simply being present and offering quiet support can make a difference. You don’t need to talk constantly; just sitting together or watching a movie together can provide comfort.

Encourage self-care: Suggest light activities like short walks or breathing exercises. If they can’t eat heavy meals, ensure they are still nourished by providing semi-solid foods like juices, soups, smoothies, or fresh fruits. Help maintain a regular sleep schedule by encouraging a consistent bedtime and wake-up time. Encourage them to continue doing small, manageable tasks to create a sense of accomplishment.

Helpful statements for depressive episodes: “I’m here for you. We can just sit together if that makes you feel better.”
“Would you like to watch your favourite movie or play a game? We can make some popcorn too.”
“It’s okay to feel this way. You’re not alone in this. I’m here to support you, no matter how long it takes.”
“Let’s set a small goal for today, like getting out of bed or taking a shower. We can celebrate these little victories together.”
Holistic support for individuals with bipolar disorder and their families: Mental Health Support Foundation
Professional guidance can provide more comprehensive support. Feel free to share the contact information for our Free Counselling Helpline service with your care-recipient. Our helpline number is 8686139139, and operates every day of the week from 9am to 8pm. Additionally, to receive 1-to-1 appointment based online therapy, they can book the session by clicking on link.
Anxiety disorders are characterized by excessive worry, fear, or anxiety that interferes with daily activities.
To learn more about anxiety, visit https://www.manntalks.org/anxiety/

Engage in deep breathing exercises: Help your loved one manage anxiety by guiding them through deep breathing exercises. This exercise can create a calm atmosphere and encourage relaxation. Example: “Let’s take a few deep breaths together. Inhale deeply through your nose, hold for a moment, exhale slowly through your mouth, and again hold for a few moments.

Encourage calming activities: Recommend simple, soothing activities like listening to music, taking a walk, or practicing mindfulness. These can be effective in managing anxiety and breaking the anxiety cycle.



Here is a guide to support someone experiencing panic attacks: https://www.manntalks.org/anxiety/panic-attacks/
Depression is characterised by persistent feelings of sadness and loss of interest in activities that were once enjoyable.
To know more about the symptoms, click here.
It is important to understand that depression is not sadness. Unlike feelings of sadness, which can often be alleviated in a matter of days, overcoming depression requires long-term care and support. Those dealing with depression may struggle to function in their daily lives, and it can become challenging for them to take care of themselves.
Being depressed is not a choice, it is an extremely exhausting condition and may take months if not years to get better. Supporting individuals going through depression can mean acknowledging what they are going through and providing the necessary support they need.


Humans naturally mirror each other’s emotional states, a phenomenon influenced by mirror neurons in the brain. This ability allows us to absorb and subconsciously reflect the emotions of those around us. While this can sometimes intensify distress in challenging situations, a caregiver can intentionally harness emotional mirroring to support and uplift their care-recipient, helping them feel safe, motivated, and hopeful.
For instance, when the care-recipient is upset or frustrated, the caregiver can maintain steady breathing, speak in a gentle tone, and adopt relaxed body language. These cues subconsciously signal calmness, encouraging the care-recipient to feel more at ease. Sharing positive yet realistic perspectives and expressing confidence in their ability to handle challenges can further build resilience and trust. Additionally, celebrating small victories or sharing moments of gratitude can foster a sense of accomplishment and connection.
Engaging in grounding techniques, such as deep breathing, mindfulness, alongside the care-recipient can be more effective than merely suggesting they do these activities independently. This shared approach not only demonstrates support but also reinforces the caregiver’s role as a calming and motivating presence.
If the care-recipient talks about ending their life, here is the guide for you: https://www.manntalks.org/helping-someone/gatekeeping/
Consistent support through therapy is one of the essential elements in managing this disorder. You can share the contact information of our Free Counselling Helpline service with your care-recipient. Our helpline number is 8686 139139, and it operates every day of the week from 9am to 8pm. Additionally, to receive a 1-to-1 appointment- based online therapy, they can book the session by clicking on this link.
Schizophrenia is a serious mental disorder characterised by distorted thinking, perceptions, emotions, language, and sense of self. They have difficulty figuring out what is real v/s what is not.

Set Up a Relaxation Space: Designate a peaceful area in the home where they can retreat when feeling overwhelmed. Remove any sharp objects and minimise bright lights or any loud noises around the room. This could be a bedroom set up with pillows and blankets to create a soothing and safe atmosphere. For example, you could say, “Let’s set up this cosy corner where you can relax whenever you need to.”



For holistic support for a care-recipient with schizophrenia and their family, visit the Schizophrenia Research Foundation (SCARF).
Substance use disorder is characterised by an inability to control the use of legal or illegal drug, leading to significant impairment or distress in day-to-day life.
A lot of people believe that individuals with substance abuse problems just don’t want help. However, the truth is, that many feel trapped by their addiction and are weighed down by shame, fear, or uncertainty about how to seek assistance. It’s also important to remember that while using substances may start as a choice, addiction fundamentally alters brain chemistry, making it incredibly challenging for individuals to regain control.
Similarly, there’s this idea that recovery is a quick and easy journey, but it’s often far from that-setbacks and relapses are common, and real change takes a long-term commitment. Lastly, the stereotype that people going through addiction are dangerous can be harmful; many people struggling with substance use are just trying to navigate their challenges and deserve understanding and compassion, not judgement.





The Mann Talks Helpline employs trained mental health professionals who offer an empathetic and non-judgemental environment where you can share your thoughts, emotions and experiences freely. The conversation will be confidential, and your privacy will be respected at all times.
Calling the Mann Talks helpline offers:
We are an inclusive platform and encourage individuals from across experiences, backgrounds and abilities to use the services available. We do not discriminate on any grounds, whatsoever.
A common misconception is that a helpline should only be used in moments of crisis. You can reach out to Mann Talks any time you are feeling emotionally distressed.
We often feel guilty about reaching out to friends and family constantly. We fear their judgement, or we may not want to share sensitive information with those close to us. At Mann Talks, you will get to speak to a trained mental health professional who will provide you with an unbiased, safe and confidential space where you can comfortably share your thoughts, emotions and experiences.
Sometimes, a loved one may be going through a tough time and you may not know how to help them. You can reach out to Mann Talks on behalf of your loved one to find out how to support them and minimize the emotional distress they are going through.
When you call the helpline, the mental health professional that you speak to will be respectful, emotionally supportive, non-judgmental and listen to you patiently.
At Mann Talks, we consider privacy and confidentiality to be of utmost importance. We prioritize our callers' privacy so that their identity, respect and dignity are uncompromised.
All conversations between the caller and our mental health professionals will remain confidential unless there is danger to the callers or others.
All conversations between the caller and our mental health professionals will remain confidential unless there is danger to the caller or others.The trained mental health professionals speak in Hindi, Marathi, Punjabi, Bengali and English. The Helpline is active from Mon-Sun, 9 a.m. to 6 p.m.
While talking to a friend or family member may be comforting, there is a risk that they might bring their own biases and judgements to the conversation. There may also be things that we don’t want our loved ones to know—thoughts and emotions that cause us anxiety, guilt or shame; or painful emotions that they might not be able to handle.
The mental health professionals at Mann Talks are trained in the art of listening and offer a safe space without any bias or judgement. This will allow you to speak more freely than you would with someone you know. They are also trained to be able to understand your pain and situation, and help you resolve your issues.
At Mann Talks, we prioritize confidentiality, dignity and respect of the caller. Our mental health professionals will not share anything you discuss with anyone else. The only time confidentiality may be broken is if the mental health professional feels you might harm yourself, or those around you.
In any other circumstance, what you share remains confidential.
It is important to feel comfortable with the mental health professional you’re accessing treatment from. If you feel like the professional you’ve been assigned/are speaking to isn’t a good fit for you, it’s okay to request a different one.
Don’t feel pressured to continue to talk to a professional you don’t like—after all, Mann Talks is for your wellbeing, and your comfort comes first.






